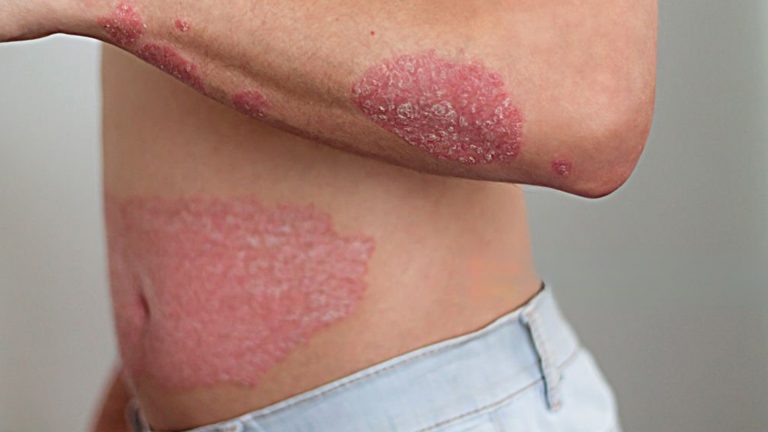
Resistant fungal skin infections have become a formidable challenge in clinical dermatology. These infections, caused by a variety of pathogenic fungi, can be incredibly stubborn to treat due to the emergence of resistance to commonly used antifungal medications. Understanding the causes, risk factors, and management of these resistant fungal skin infections is crucial for effective treatment.
Causes of Resistance
The development of resistance in fungal skin infections can be attributed to several factors:
- Overuse or Misuse of Antifungal Agents: The over-prescription and inappropriate use of antifungal medications have exerted selective pressure on fungi. This pressure leads to the survival and proliferation of resistant strains, making treatment more difficult.
- Incomplete Treatment Courses: Stopping antifungal treatment prematurely, often when symptoms subside, can allow surviving fungi to develop resistance and resurge. Completing the full course of treatment is essential.
- Non-Adherence to Prescribed Regimens: Patients who do not adhere to their prescribed treatment regimens are more likely to develop resistance. Failure to take medications as directed or applying topical treatments irregularly can lead to inadequate control of the infection.
- Intrinsic Resistance: Some fungi, such as Trichophyton rubrum, have shown inherent or intrinsic resistance to certain antifungal agents. This means that even with proper use, these medications may not be effective against these particular fungi.
Risk Factors
Several risk factors increase the likelihood of developing resistant fungal skin infections:
- Immunocompromised Status: Individuals with compromised immune systems, such as those with HIV/AIDS or organ transplant recipients, are at a higher risk of developing resistant fungal skin infections. Their weakened immune response makes it easier for fungi to establish resistance.
- Underlying Medical Conditions: Conditions like diabetes and chronic corticosteroid use weaken the body’s natural defenses against fungal infections. This makes individuals with these conditions more susceptible to developing resistant infections.
- Recurrent Infections: Individuals who experience recurrent fungal skin infections may be more prone to resistance. Repeated infections can create an environment where resistant fungal strains can thrive.
- Infection Location: Infections in areas such as the nails, scalp, or mucous membranes can be harder to treat due to reduced drug penetration. The location of the infection can impact the effectiveness of treatment.
Management
Effectively managing resistant fungal skin infections requires a multi-faceted approach. Here are some strategies to consider:
- Comprehensive Assessment: A thorough clinical and mycological assessment is crucial. Identifying the causative fungus, its susceptibility to antifungals, and resistance mechanisms can guide treatment decisions.
- Alternative Antifungal Agents: When resistance is suspected or confirmed, switching to antifungal agents from a different class can be effective. These alternative agents may be more successful in combating the resistant strain.
- Combination Therapy: In some cases, combining two or more antifungal agents can enhance treatment efficacy. This strategy may help overcome resistance and improve outcomes.
- Adjunctive Therapies: Depending on the severity and location of the infection, topical or systemic adjunctive therapies such as photodynamic therapy or immunomodulators may be considered to augment the antifungal treatment.
- Patient Education: Educating patients about the importance of adherence to treatment regimens, personal hygiene, and lifestyle modifications is crucial. Reinforce the necessity of completing the full course of treatment and maintaining good hygiene to prevent reinfection.
- Preventive Measures: Implementing infection control practices, such as proper wound care and hygiene, can help reduce the risk of resistance. Encouraging patients to avoid sharing personal items that may harbor fungi, such as towels or shoes, is essential.
In conclusion, the emergence of resistant fungal skin infections is a growing concern in dermatology. Effective management necessitates a comprehensive approach, including accurate diagnosis, susceptibility testing, and the selection of appropriate antifungal therapies. It is crucial for both healthcare providers and patients to work together to mitigate the risk of resistance and ensure successful treatment outcomes. By understanding the causes and risk factors, and by implementing these management strategies, we can better combat resistant fungal skin infections and provide relief to patients suffering from these challenging conditions.